|
|
Case Report
| ||||||
| A rare case of Type III gastric volvulus: Presentation and laparoscopic management | ||||||
| Simeon Ngweso1, Anand Trivedi2, Senarath Werapitiya3 | ||||||
|
1B.Pharm, MBBS, Resident Medical Officer, Surgical Department, Royal Perth Hospital, Perth, Western Australia, Australia.
2MBBS, MS (General Surgery), Advanced General Surgical Registrar, General Surgery Department, Bunbury Regional Hospital, Bunbury, Western Australia, Australia. 3MBBS, MS, FRCS, FRACS, General Surgery Consultant/Upper GI Consultant, General Surgery Department, Bunbury Regional Hospital, Bunbury, Western Australia, Australia. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Ngweso S, Trivedi A, Werapitiya S. A rare case of Type III gastric volvulus: Presentation and laparoscopic management. J Case Rep Images Surg 2016;2:101–104. |
|
Abstract
|
|
Introduction:
Gastric volvulus is a surgical emergency and a recognized complication of hiatal hernia. Type III gastric volvulus is the rarest variant and is characterized by gastric rotation about both the organoaxial and mesenterioaxial axes. Presentation and management of Type III gastric volvulus is not well described in literature.
Case Report: An 89-year-old male presented with eight hours of coffee-ground vomiting. The patient was hemodynamically stable and examination was unremarkable. Imaging confirmed a large gastric volvulus. Gastric decompression was performed endoscopically and laparoscopy confirmed a huge Type III gastric volvulus with complex rotation of the stomach about both the organoaxial and mesenterioaxial axes. The stomach and distal esophagus were laparoscopically mobilized to ensure adequate intra-abdominal esophageal length. Due to the very large diaphragmatic defect, crural opposition was not possible so the stomach was fixed laparoscopically via gastropexy from the anterior abdominal wall to the diaphragm. The patient made an uneventful postoperative recovery. Three months follow-up confirmed no recurrent symptoms. Conclusion: Gastric volvulus is rare but life-threatening. Type III gastric volvulus is the rarest variant with limited description in literature. In this particular case, endoscopic decompression and laparoscopic reduction and fixation without fundoplication was a successful treatment modality. | |
|
Keywords:
Gastric volvulus, Laparoscopic surgery, Laparoscopic management
| |
|
Introduction
| ||||||
|
Gastric volvulus is a recognized complication of hiatal hernia and is characterized by abnormal rotation of the stomach by more than 180° resulting in a luminal obstruction [1]. Gastric volvulus is a rare disease with an unknown incidence primarily because the condition can occur in an acute or chronic variant [2]. Considered a surgical emergency, gastric volvulus has a non-operative mortality rate potentially as high as 80% [1] [3]. Type I or organo-axial gastric volvulus accounts for 60% of gastric volvulus and is characterized by the stomach rotating around its long axis [1]. Type II or mesenterioaxial volvulus occurs with rotation of the stomach along an axis perpendicular to its longitudinal axis [3]. In Type II volvulus, the stomach typically lies in a vertical plane, with the antrum and pylorus rotated anterior and superior to the gastroesophageal junction [3]. Almost 30% of cases are Type II gastric volvulus [2]. Rotation of the stomach about both the organoaxial and mesenterioaxial axes is a Type III or "combined volvulus" [1]. Type III volvulus is extremely rare, potentially only comprising 12% of all cases of gastric volvulus [2]. Due to its rarity, the presentation and management options of particularly Type III gastric volvulus is not well described in literature. | ||||||
|
Case Report
| ||||||
|
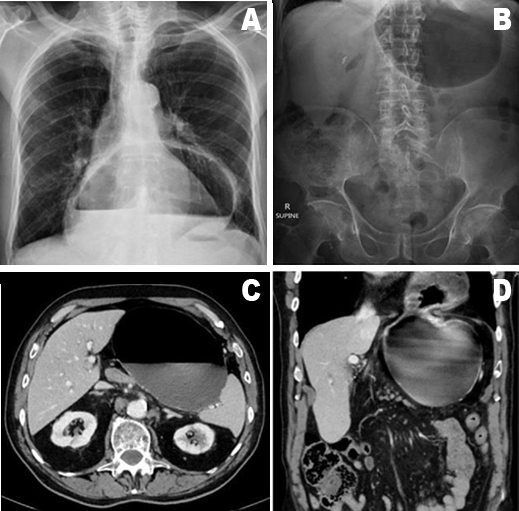
An 89-year-old male presented to the emergency department with an eight hour history of coffee-ground vomiting. There was no associated abdominal pain or significant abdominal distension. No bowel changes, no fevers, no weight loss or night sweats and the patient had been well otherwise. The patient had a history of reflux, and was on a proton-pump inhibitor, had hypertension, hypercholesterolaemia and had undergone a previous open cholecystectomy. There was no history of malignancy or previous endoscopy. Upon presentation, the patient was hemodynamically stable and examination was unremarkable with a soft, non-peritonitic abdomen and no significant findings. Initial abdominal and chest X-ray revealed a large hiatus hernia and follow-up computed tomography scan of abdomen confirmed the presence of a large, Type III gastric volvulus (Figure 1). The patient was subsequently transferred to a larger, close-by hospital with surgical and endoscopic capabilities where he underwent urgent operative assessment. Gastroscopy and gastric decompression was performed with large amounts of hemorrhagic gastric contents being aspirated. Gastroscopy revealed early ischemic changes of the gastric mucosa and confirmed a huge hiatus hernia with complex rotation of the stomach about both the organoaxial and mesenterioaxial axes. All contents of the mixed type volvulus were viable. The stomach and distal esophagus were laparoscopically mobilized to ensure adequate intra-abdominal esophageal length. Due to the very large diaphragmatic defect, crural opposition was not possible so the stomach was fixed laparoscopically via gastropexy from the anterior abdominal wall to the diaphragm using multiple sutures and small Vypro mesh patches to facilitate the formation of adhesions and prevent recurrence (Figure 2). Postoperatively, the patient was admitted to the high dependency unit for a period of observation. He was subsequently transferred to the general surgery ward where he remained for one week undergoing physiotherapy and being treated with DVT prophylaxis, analgesia and empirical antibiotics for potential aspiration. Once clinically stable and after being cleared by allied health, the patient was successfully discharged home. After three months follow-up, the patient has denied any major reflux symptoms or post-prandial early satiety. | ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
Gastric volvulus is a potential complication of hiatus hernia and is characterized by abnormal rotation of the stomach by more than 180° [1]. Gastric volvulus was first described in 1866 by Berti, based on the autopsy of a 61-year-old woman [3]. Gastric volvulus is a rare condition that can prove to be a diagnostic dilemma; However, it is life-threatening and requires prompt diagnosis and treatment as delay can result in obstruction, incarceration, perforation and ultimately death [3] [4]. Treatment of gastric volvulus involves decompression, reduction and prevention of recurrence with laparoscopic or open repair providing the mainstays of interventional therapy [3] [5]. Laparoscopic repair has proven to be feasible and safe and provides the standard approach in many centers [1] [6]. Fundoplication has been suggested as a mandatory part of operative management as it prevents reflux and provides a good anchor for the repair [6]. However, following a recent retrospective review of cases, Light et al. concluded that in a frail elderly patient with a large hiatal defect, consideration may be given to reducing the stomach with fixation via anterior abdominal and diaphragmatic gastropexy without hiatal repair [7]. Good outcomes were found with both gastropexy with or without fundoplication with the decision dependent on factor including the status of the patient during surgery and integrity of the stomach [7]. Similarly, a review of a case series by Yates et al. determined that for surgeons not comfortable performing an urgent laparoscopic gastric hernia repair, laparoscopic gastropexy is a technically less challenging operation that can alleviate acute gastric volvulus and relieve gastric outlet obstruction [8]. Laparoscopic gastropexy without fundoplication also facilitates successful treatment of the acute obstruction while allowing referral to a tertiary centre where definitive hiatal repair can occur if necessary and also reduces operative time which is beneficial for patients at high surgical risk [8]. There is, however, limited information regarding the management options pertaining specifically to Type III gastric volvulus. Similar to accepted practice for other forms of gastric volvulus, a management approach implementing decompression, reduction and fixation would be considered appropriate and in this particular case proved to be successful. | ||||||
|
Conclusion
| ||||||
|
Gastric volvulus, particularly the Type III variant, is a rare surgical emergency. Endoscopic decompression with laparoscopic reduction is a viable treatment modality. Fundoplication is generally recommended, however, fixation via anterior abdominal and diaphragmatic gastropexy without fundoplication is acceptable in a frail, elderly patient with a large defect. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Simeon Ngweso – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Anand Trivedi – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Senarath Werapitiya – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Simeon Ngweso et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|