|
|
Case Report
| ||||||
| Massive splenic artery aneurysm with aneurysmal dilatation of the portal vein and splenic infarct | ||||||
| Samrat Ray1, Amitabh Yadav1, Samiran Nundy1 | ||||||
|
1Department of Surgical Gastroenterology and Liver Transplantation, Sir Ganga Ram Hospital, Rajinder Nagar, New Delhi.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Ray S, Yadav A, Nundy S. Massive splenic artery aneurysm with aneurysmal dilatation of the portal vein and splenic infarct. J Case Rep Images Surg 2017;3:1–5. |
|
Abstract
|
|
Introduction:
Aneurysms of the splenic artery are rare but potentially life-threatening problems and the risk of complications increases manifold with their increase in size. The portal vein aneurysms are even rarer with as few as only 200 cases being reported in the surgical literature. The presence of both aneurysms in the same patient has not been previously described. Such cases present a therapeutic challenge.
Case Report: A 56-year-old apparently healthy male presented with vague upper abdominal discomfort with fever, headache and a palpable spleen. Evaluation by triple phase computed tomography of the abdomen revealed a large 9×8 cm sized aneurysm in the distal third of the splenic artery with an aneurysmal dilatation of the portal vein about 48 mm at the porta hepatis, splenomegaly with a splenic infarct and multiple gallstones. Laparotomy with distal pancreatosplenectomy, excision of the aneurysm and cholecystectomy were done. Gross evaluation of the specimen revealed a 10 cm aneurysm of the distal splenic artery containing organised thrombus within an infarct at the lower pole of the spleen. Conclusion: Presentation of a massive splenic artery aneurysm in association with a portal vein aneurysm is an exceedingly rare clinical phenomenon. Most portal vein aneurysms being asymptomatic may be left alone and followed up periodically. We describe an extremely rare association of coexistent aneurysms of the splenic artery and portal vein which was managed by distal pancreatectomy and splenectomy. | |
|
Keywords:
Aneurysm, Portal vein aneurysm, Splenic artery aneurysms
| |
|
Introduction
| ||||||
|
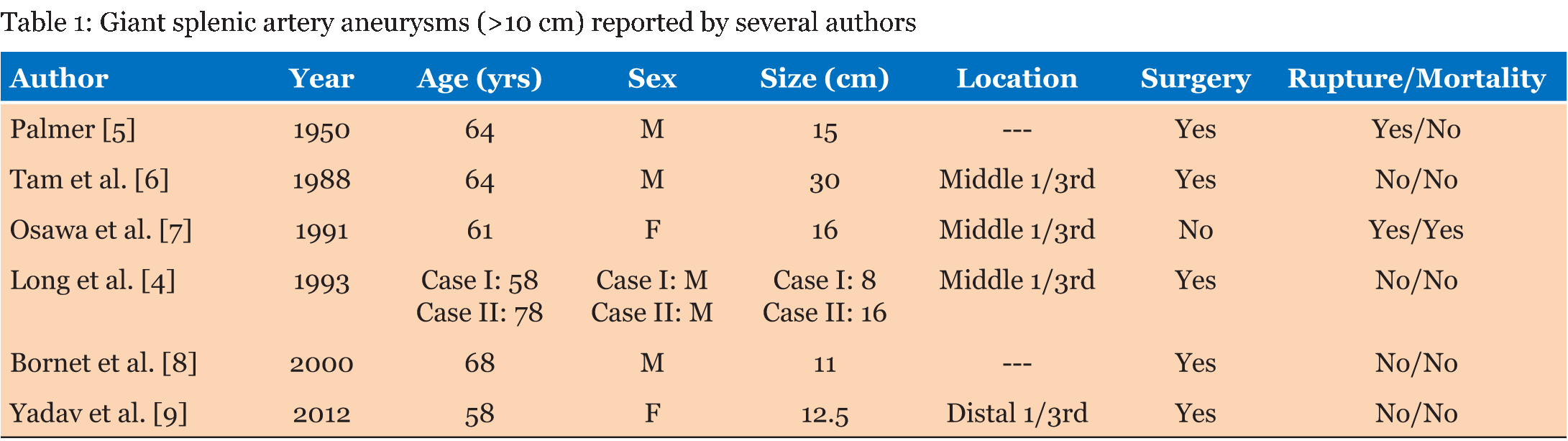
Aneurysms of the visceral arteries are rare but potentially life-threatening. The splenic artery accounts for the majority of splanchnic artery aneurysms, comprising 60–70% of the total cases detected [1]. Splenic artery aneurysms (SAA) also represent the third most common site of intra-abdominal aneurysms, preceded by aorta and the iliac arteries [2]. Rupture of the aneurysm constitutes the major risk and size is the most important determinant to predict the likelihood of rupture [3]. Splenic artery aneurysms rarely exceed 3 cm in diameter [4]. Table 1 gives an overview of the giant splenic artery aneurysms (>10 cm) reported so far by several authors [4] [5] [6] [7][8][9]. A rare but fatal mode of presentation of SAAs is in the form of spontaneous rupture, reported in 2–10% of the cases. The risk of rupture in giant aneurysms is reported to be around 28%, with an attendant mortality of around 40% [3]. The earliest description of portal vein aneurysm (PVA) in the surgical literature dates back to 1956, with the earliest description of this disease entity by Barzilai and Kleckner in a 21-year-old white female presenting with massive gastrointestinal bleeding. Since then, there have been more than 200 cases described so far in the surgical literature from all over the world. Portal vein aneurysm is defined as abnormal aneurysmal dilatation of the vein (>1.9 cm in cirrhotic livers and >1.5 cm in non-cirrhotic livers) [10]. The incidence of portal vein aneurysm is only about 0.06% [11]. The association of incidentally detected PVA in a patient with a massive SAA makes an exceedingly rare clinical scenario and to our knowledge, has not been described so far. We present a case of a middle aged healthy man with a giant splenic artery aneurysm associated with an aneurysmal dilatation of the portal vein and splenic infarct. | ||||||
| ||||||
|
| ||||||
|
Case Report
| ||||||
|
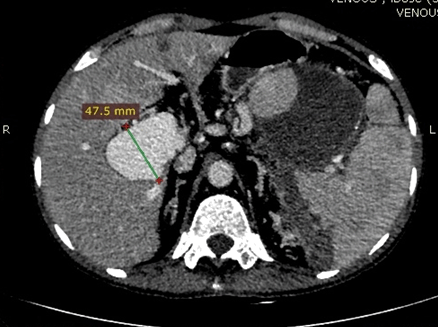
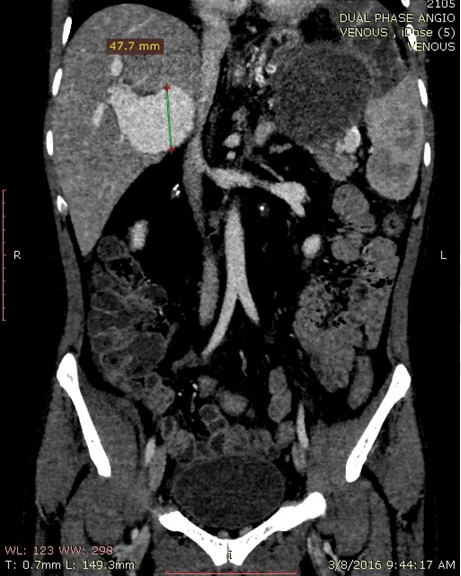
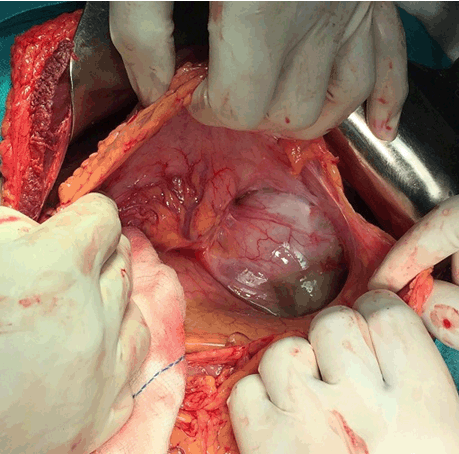
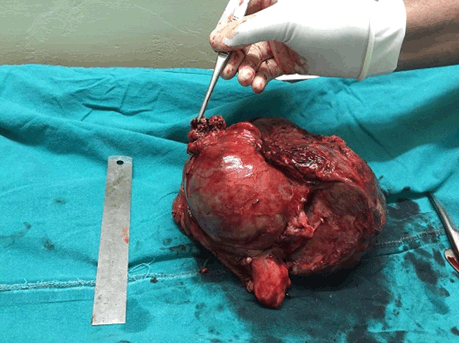
A 56-year-old male with no known medical comorbidity presented with complaints of vague upper abdominal discomfort associated with nonspecific left sided headache for one month and fever on and off for 15 days. On examination, he was conscious, comfortable and cooperative with a blood pressure of 130/70 mmHg and a pulse rate of 84/min. On abdominal examination, there was fullness in the epigastrium with tip of the spleen palpable below the left costal margin. Computed tomography angiography of the abdomen revealed a large heterogeneous mass near the splenic hilum measuring around 9×8.3 cm in the axial plane and approximately 8.6 cm in its craniocaudal extent in relation to the tail of pancreas bulging into the lesser sac and abutting the greater curvature of stomach with faint contrast uptake along the periphery with another large hyperdense mass within, consistent with a large splenic artery aneurysm containing a thrombus (Figure 1). On the arterial phase scan, there was minimal enhancement within this lesion. The spleen was enlarged with an infarct in its lower pole. The liver was grossly normal with no nodularity. There was an aneurysmal dilatation of the portal vein at the porta hepatis, measuring 47.7 mm in the largest diameter (Figure 2). The patient underwent laparotomy with a distal pancreatosplenectomy with resection of the splenic artery aneurysm with cholecystectomy. There was a large pulsatile lesion measuring approximately 10×9 cm along its largest dimensions compressing the distal pancreas posteriorly and a part of the greater curvature of the stomach anterosuperiorly (Figure 3). The portal vein was dilated, measuring 4×3.5 cm. The pulsatile lesion was controlled by identifying the splenic artery and placing a vascular clamp across it. The splenic artery and vein were ligated, transfixed and divided and the specimen was removed. Cholecystectomy was also done. The gross specimen showed a 10×9.5 cm large aneurysmal sac adherent to the splenic hilum with a large clot present within (Figure 4). The spleen was engorged with an infarct localised to the lower pole. Microscopic analysis revealed marked intimal thickening of the splenic artery with fibrosis and focal calcification of the aneurysm wall. The postoperative course was uneventful and the patient was discharged in stable condition on day-7 following surgery. | ||||||
| ||||||
|
| ||||||
| ||||||
| ||||||
|
Discussion
| ||||||
|
The prevalence of true splenic artery aneurysms has been estimated to be around 0.1% [3]. The majority of these aneurysms are detected incidentally and in a series from the Mayo clinic, 90% of the patients were asymptomatic at the time of presentation [12] . The symptoms of SAAs are variable, the most common being upper abdominal pain, similar to that in the present case. A catastrophic complication is spontaneous rupture; the incidence of which increases with pregnancy, size >2 cm, the presence of portal hypertension and previous portacaval shunt operations or liver transplantation [13]. The usual location of the aneurysm is in the middle or distal third of the splenic artery, close to its bifurcation [3]. Secondary calcification of the aneurysm or formation of embolus causing a block in the distal splenic microcirculation may be the presumed causes of development of splenic infarcts. In the present case also, the spleen was found to contain an evolving infarct in its lower pole. Another interesting finding in this case was the incidental discovery of a portal vein aneurysm (4.7 cm) in addition to the splenic artery aneurysm. The congenital variant is hypothesized to be a result of an incomplete regression of the right primitive distal vitelline vein [14]. The acquired variant most commonly may be secondary to portal hypertension. The usual location of these aneurysms is in the main trunk of the portal vein or near the bifurcation. In this case, it was located at the porta hepatis. In a systematic literature search by Laurenzi et al. [10], there were 96 reports identified from 1956 to 2014, which included 190 patients with portal vein aneurysm. Most of the cases were discovered incidentally. Though there are no defined guidelines for operation in splenic artery aneurysms, a size >2 cm is a definitive indication for intervention. The SAA in the present case was around 10 cm along the largest axis and hence was a definite candidate for operative management. The treatment options available for splenic artery aneurysms can be broadly categorized as open aneurysmectomy and endovascular treatment. Lakin et al. [15], in their series of 128 consecutive patients found the endovascular approach to be associated with a superior safety profile and a good regression of size (1.5 mm) over two years period of observation. The giant SAAs pose a challenge for the operating surgeon. The preferred incision is a matter of individual choice. Long et al. [4] in their report of two giant splenic artery aneurysms found a good surgical access using the thoracoabdominal incision, thereby gaining a retroperitoneal access to the aorta and the coeliac trunk, which might otherwise be difficult due to the location of the aneurysm. In the present case, we used a Chevron's roof top incision and found a comfortable anterior access to the lesser sac for dissection and avoided the chances of postoperative chest related complications associated with the former. Endovascular therapy for splenic artery aneurysms dates back to 1978, with the pioneer description of transcatheter embolization by Probst et al. [16]. With the advancement in the technique of intervention radiology, the success rate of these procedures approach nearly 100%. Embolization is usually performed for all SAAs except for those located near the splenic hilum, due to the high risk of splenic infarction. The procedure is associated with certain complications such as distal migration of the coil, post embolization abscess or infarct formation and rarely, rupture of the aneurysm. In SAAs with a straight course and minimal tortuosity, endovascular stent grafting is another attractive option [17]. However, less is known about the durability and the long-term patency of these grafts. They are preferred over embolization in cases where preservation of arterial access to the spleen is important, like in cases of hypersplenism or portal hypertension shunt procedures. In this case, we used a one stage open aneurysmectomy with splenectomy and distal pancreatectomy. The patient had no significant complication at the end of 30 days observation period (Clavien Dindo I/Comprehensive complication index 8.5) [18]. In the review published by Laurenzi et al., 21% of the patients underwent surgery for portal vein aneurysm and of these patients, 20% had underlying liver cirrhosis, while 10% had portal hypertension [17]. Asymptomatic PVAs can be left alone and followed-up on an OPD basis. The presence of features of portal hypertension guides the surgical approach of management. In the absence of portal hypertension, these can be managed by aneurysmectomy or aneurysmorrhaphy. In this case, the patient had no features suggestive of portal hypertension or decompensated liver functions and was therefore, managed conservatively on a follow-up basis. | ||||||
|
Conclusion
| ||||||
|
Owing to the high morbidity and mortality associated with the complications, it is important to acquire a thorough knowledge about the detailed anatomy and the surgical techniques when dealing with splenic artery aneurysms. The risk increases manifold with increase in size of these aneurysms. Portal vein aneurysms are usually an incidental finding. The presence of massive symptomatic splenic artery aneurysm with portal vein aneurysm has not been previously described to our knowledge. The management of portal vein aneurysm in such cases is on the conservative lines if asymptomatic and static. | ||||||
|
References
| ||||||
| ||||||
|
Suggested Reading
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Samrat Ray – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Amitabh Yadav – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Samiran Nundy – Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2017 Samrat Ray et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|