|
Case Series
Treatment of anterior cutaneous nerve entrapment syndrome using an ultrasound-guided transverse abdominis plane block
1 Northern Health, 185 Cooper Street, Epping, Victoria 3076, Australia
2 Division of Surgery, Anaesthesia, and Procedural Medicine, Austin Health, 145 Studley Road, Heidelberg, Victoria 3084, Australia
3 Central Gippsland Health, 155 Guthridge Parade, Sale, Victoria 3850, Australia
Address correspondence to:
Amar Lakhani
Austin Health, 145 Studley Road, Heidelberg, Victoria 3084,
Australia
Message to Corresponding Author
Article ID: 100118Z12AL2023
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Lakhani A, Strauss P, Wasserman H. Treatment of anterior cutaneous nerve entrapment syndrome using an ultrasound-guided transverse abdominis plane block. J Case Rep Images Surg 2023;9(1):13–16.ABSTRACT
Introduction: Anterior cutaneous nerve entrapment syndrome (ACNES) is increasingly being considered to be a common cause of abdominal pain. Unfortunately, ACNES is a condition that is frequently overlooked and misdiagnosed resulting in chronic abdominal wall pain, unnecessary investigations, procedures, and repeat admissions. Patients diagnosed with ACNES present with well-localized abdominal pain, a positive Carnett’s sign, somatosensory disturbance of the surrounding skin and symptomatic relief secondary to a trigger point injection. Current treatment strategies include modification of physical activity, simple analgesia, trigger point injections, chemical neurolysis, pulsed radiofrequency, and anterior neurectomy. Despite the plethora of treatment modalities, it is evident that a majority of patients will only experience temporary pain relief.
Case Series: We describe two cases in which ultrasound-guided transverse abdominal plane blocks have successfully provided long-term symptomatic relief in patients diagnosed with ACNES. The first being a 45-year-old female and the second is a 52-year-old male who both presented with ACNES which were successfully treated with an ultrasound-guided transverse abdominal plane (TAP) block with 20 mL of 0.25% Marcaine and 4 mg of Dexamethasone.
Conclusion: We provide evidence supporting the use of an ultrasound-guided TAP block for long-term symptomatic relief in patients with ACNES. However, further research is required to assess its efficacy.
Keywords: Anterior cutaneous nerve entrapment syndrome, Chronic abdominal pain, Ultrasound-guided transverse abdominal plane block
Introduction
Anterior cutaneous nerve entrapment syndrome (ACNES) is increasingly being considered to be a common cause of abdominal pain. It is estimated that 2% of patients who present to the emergency department with abdominal pain suffer from ACNES [1]. Unfortunately, ACNES is frequently overlooked and misdiagnosed resulting in unnecessary investigations, futile diagnostic procedures, repeat admissions, and significant morbidity.
The entrapment of the anterior cutaneous branch of the thoracoabdominal (T7-11) and subcostal (T12) nerves results in the development of ACNES [2],[3]. By piercing the posterior rectus sheath at 90° through a fibrous ring at the lateral border of rectus abdominus the nerve becomes susceptible to compression [2]. Entrapment of the nerve may result from increases in intra- and extra-abdominal pressure, ischemia, herniation, or scaring [4].
A thorough history and examination is essential to diagnose ACNES, in doing so excluding organic causes of abdominal pain. Anterior cutaneous nerve entrapment syndrome is a clinical diagnosis requiring the presence of well-localized abdominal pain, increased tenderness to palpation during muscle tensing on physical examination (Carnett’s sign), somatosensory disturbances of the surrounding skin, and response to a trigger point injection with local anesthetic [4].
The goal of treatment is to alleviate patient’s symptoms. Current recommendations include modification of physical activity, simple analgesia, trigger point injections with local anesthetic alone or in combination with a glucocorticoid, chemical neurolysis, pulsed radiofrequency, and anterior neurectomy [5],[6]. Despite multiple treatment strategies and modalities, it is evident that a majority of patients will only experience temporary pain relief [4]. We report two consecutive cases in which an ultrasound-guided transverse abdominal plane (TAP) block has provided long-term relief for patients suffering from ACNES.
Case Series
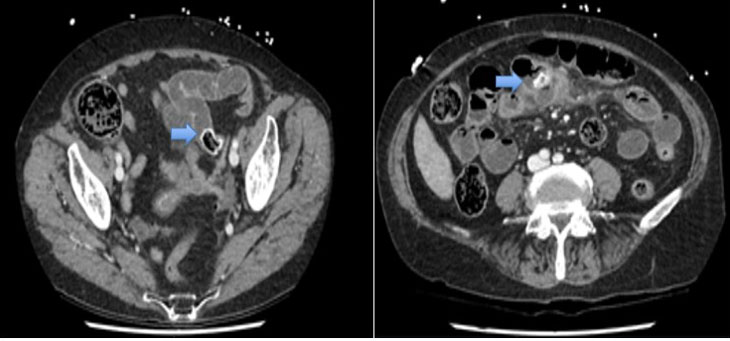
Case 1: A 45-year-old female presented to the emergency department with left upper quadrant pain for one year. The pain was described as well-localized to the lateral border of rectus abdominus. She experienced no associated symptoms. On examination a positive Carnett’s sign was elicited. Her laboratory results were unremarkable. Extensive imaging including an abdominal ultrasound, computed tomography (CT), hepatobiliary iminodiacetic acid (HIDA) scan as well as a colonoscopy and gastroscopy excluded organic causes of abdominal pain. Subsequently a trigger point injection using 10 mL of lidocaine 1% with adrenaline was performed. The patient demonstrated partial resolution of pain within 15 minutes of the procedure confirming the diagnosis of ACNES. A decision was made to proceed with an ultrasound-guided TAP block lateral to the rectus sheath for treatment of her pain. The procedure was performed under sedation. A 21-gauge 110 mm needle was used to inject 20 mL of 0.5% Marcaine with adrenaline and 4 mg of Dexamethasone into the neurovascular plane (Figure 1). She required a repeat TAP at six weeks and has been symptom free for six months.
Case 2: A 52-year-old male presented to clinic with a 3-month history of well-localized left upper quadrant pain located at the lateral border of the rectus muscle. The patient had no associated symptoms. Carnett’s sign was demonstrated on physical examination. The diagnosis of ACNES was confirmed with the transient resolution of symptoms 24 hours post-trigger point injection. An ultrasound-guided TAP block was performed in an attempt to relieve his symptoms. Intravenous sedation was used prior to injecting 20 mL of 0.25% Marcaine and 4 mg of Dexamethasone into the neurovascular plane using a 21-gauge 110 mm needle. Complete resolution of the patient’s symptoms was observed at six months follow-up.
Discussion
By injecting local anesthetic in a plane between internal oblique and transverse abdominus one is able to block the neuronal afferent fibers of thoracoabdominal (T7-11) subcostal (T12) nerves (Figure 2) [7],[8]. Transverse abdominal plane blocks have become technically easier and safer given the ubiquity of ultrasound and skilled practitioners who are qualified to perform the procedure. It provides a safe and viable option for the management of abdominal wall pain. Despite its increasing use for acute pain management in abdominal and pelvic procedures minimal research has been performed assessing its efficacy in the treatment of somatic pain syndromes such as ACNES.
To date there are only two case reports demonstrating the efficacy of TAP blocks for the treatment of ACNES [9],[10]. Imajo et al. highlighted the case of a 56-year-old male diagnosed with ACNES following a cholecystectomy who was initially managed with an ultrasound-guided rectus sheath block to partial effect [9]. To further alleviate his pain an ultrasound-guided bilateral TAP block with 20 mL of 0.5% mepivacaine was used successfully [9]. Sahoo et al. were also able to demonstrate the successful implementation of an ultrasound-guided TAP block for the treatment of ACNES in two patients [10].
Current treatment strategies for the management of ACNES have demonstrated poor long-term outcomes. Trigger point injections have become the gold standard for the diagnosis and treatment of ACNES. Local anesthetic (1–3 mL of lidocaine) alone or combined with a glucocorticoid (40 mg of triamcinolone) is injected into the subcutaneous tissue of the affected site. Immediate pain relief is observed in up to 91% of cases; however, commonly reoccurs in 2–3 hours [4]. Chemical neurolysis is recommended in patients who have failed treatment following a trigger point injection. A cohort of 44 patients who underwent chemical neurolysis demonstrated complete, partial, and no response in 54%, 40%, and 6% of patients [11]. Patients with partial and no response may be suitable for an anterior neurectomy. A 50% reduction in pain intensity was observed ion 61% of patients with a mean follow-up period of 32 months [12]. Limited data are available regarding the efficacy of pulsed radiofrequency, modification of physical activity, and the use of nonsteroidal anti-inflammatory medications.
Despite the multitude of treatment modalities, it is evident that none provide an effective long-term resolution to the management of ACNES. Hence, one must reconsider the treatment algorithm for the management of ACNES. We have demonstrated ultrasound-guided TAP block as a potential cost effective, efficacious, and safe procedure in the hands of a skilled physician for the treatment of ACNES. Therefore, we suggest that this case series prompts further research for the use of TAP blocks for the management of ACNES.
Conclusion
Despite its prevalence ACNES is quite often overlooked as a diagnosis for abdominal pain. An index of suspicion is imperative to avoid unnecessary investigations and procedures. Once diagnosed, there are a myriad of treatment strategies that can be used to treat ACNES. We provide evidence supporting the use of an ultrasound-guided TAP block for long-term symptomatic relief in patients with ACNES. However further research is required to assess its efficacy.
REFERENCES
1.
van Assen T, Brouns JAGM, Scheltinga MR, Roumen RM. Incidence of abdominal pain due to the anterior cutaneous nerve entrapment syndrome in an emergency department. Scand J Trauma Resusc Emerg Med 2015;23:19. [CrossRef]
[Pubmed]

2.
3.
Clarke S, Kanakarajan S. Abdominal cutaneous nerve entrapment syndrome. Continuing Education in Anaesthesia Critical Care & Pain 2015;15(2):60–3. [CrossRef]

4.
Meyer GW. Anterior cutaneous nerve entrapment syndrome. UpToDate 2023. [Available at: https://www.uptodate.com/contents/anterior-cutaneous-nerve-entrapment-syndrome?search=anterior%20cutaneous%20nerve%20entrapment&source=search_result&selectedTitle=1~124&usage_type=default&display_rank=1

5.
Maatman RC, Steegers MAH, Boelens OBA, et al. Pulsed radiofrequency or anterior neurectomy for anterior cutaneous nerve entrapment syndrome (ACNES) (the PULSE trial): Study protocol of a randomized controlled trial. Trials 2017;18(1):362. [CrossRef]
[Pubmed]

6.
Chrona E, Kostopanagiotou G, Damigos D, Batistaki C. Anterior cutaneous nerve entrapment syndrome: Management challenges. J Pain Res 2017;10:145–56. [CrossRef]
[Pubmed]

7.
Tsai HC, Yoshida T, Chuang TY, et al. Transversus abdominis plane block: An updated review of anatomy and techniques. Biomed Res Int 2017;2017:8284363. [CrossRef]
[Pubmed]

8.
Mavarez AC, Ahmed AA. Transabdominal Plane Block. 2022 Oct 3. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023.
[Pubmed]

9.
Imajo Y, Komasawa N, Fujiwara S, Minami T. Transversus abdominal plane and rectus sheath block combination for intractable anterior cutaneous nerve entrapment syndrome after severe cholecystitis. J Clin Anesth 2016;31:119. [CrossRef]
[Pubmed]

10.
Sahoo RK, Nair AS. Ultrasound guided transversus abdominis plane block for anterior cutaneous nerve entrapment syndrome. Korean J Pain 2015;28(4):284–6. [CrossRef]
[Pubmed]

11.
McGrady EM, Marks RL. Treatment of abdominal nerve entrapment syndrome using a nerve stimulator. Ann R Coll Surg Engl 1988;70(3):120–2.
[Pubmed]

12.
van Assen T, Boelens OB, van Eerten PV, Perquin C, Scheltinga MR, Roumen RM. Long-term success rates after an anterior neurectomy in patients with an abdominal cutaneous nerve entrapment syndrome. Surgery 2015;157(1):137–43. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Amar Lakhani - Conception of the work, Design of the work, Acquisition of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Paul Strauss - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Henry Wasserman - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2023 Amar Lakhani et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.