|
Case Report
Delayed presentation of gallstone ileus due to spilled gallstones: A case report
1 MBChB, General Surgical Registrar, North Shore Hospital, Auckland, New Zealand
2 MBBS, MSc, General Surgical Registrar, Monash Health, Victoria, Australia
3 MBChB, Radiology Registrar, North Shore Hospital, Auckland, New Zealand
4 MBBS, FRACS, General Surgical and Colorectal Fellow, Monash Health, Victoria, Australia
Address correspondence to:
Binura Buwaneka Wijesinghe Lekamalage
MBChB, General Surgical Registrar, North Shore Hospital, Auckland,
New Zealand
Message to Corresponding Author
Article ID: 100126Z12BL2023
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Lekamalage BBW, Thaveenthiran P, Ghate KN, Arachchi A. Delayed presentation of gallstone ileus due to spilled gallstones: A case report. J Case Rep Images Surg 2023;9(2):27–31.ABSTRACT
Introduction: Gallstone ileus is a rare cause of intestinal obstruction and very few cases have been reported of spilled gallstones during a cholecystectomy resulting in a delayed presentation of gallstone ileus. Although complications from unretrieved gallstones are rare, there is a variety of post-operative complications described in the literature. Most complications occur within the first few months but can occur up to 10 years after the procedure. If complications arise, they may lead to significant morbidity and management may result in an invasive intervention, including a laparotomy.
Case Report: An 83-year-old female underwent laparoscopic cholecystectomy for acute cholecystitis, during which several large gallstones spilled and an attempt at retrieval was made. Six years later, she presented to the emergency department with a small bowel obstruction due to gallstone ileus caused by an unretrieved spilled gallstone. She underwent laparotomy, and the gallstone was retrieved from the terminal ileum.
Conclusion: Gallstone ileus can occur because of unretrieved spilled gallstones from a cholecystectomy. Although complications from unretrieved gallstones are rare, this case report highlights the importance of considering this as a differential diagnosis when patients present with symptoms consistent with intestinal obstruction after a cholecystectomy. It is important to attempt to retrieve spilled gallstones during cholecystectomy, but if this is not feasible, this should be documented, and patients should be informed of the potential risks of unretrieved stones although rare.
Keywords: Gallstone, Gallstone ileus, Laparoscopic cholecystectomy
Introduction
Gallstone ileus is an uncommon cause of intestinal obstruction with increased prevalence in the older population [1] There are higher mortality rates in patients with gallstone ileus due to delayed diagnosis [2]. Very few cases have been reported where unretrieved spilled gallstones during a cholecystectomy have resulted in a delayed presentation of gallstone ileus.
Case Report
An 83-year-old female presented to the hospital in August 2016 with one-day history of right upper quadrant pain, vomiting, and raised inflammatory markers. She had a past medical history of diverticular disease and hypertension. Previous abdominal operations included a laparoscopic appendicectomy. She initially underwent a computed tomography (CT) scan confirming acute cholecystitis with a significantly distended gallbladder measuring 21 cm, containing multiple large gallstones (Figure 1A). An incidental finding of a 13 mm right adrenal lesion was also reported on the scan with recommendation for follow-up imaging. A subsequent ultrasound scan confirmed multiple large gallstones with pericholecystic fluid, normal ducts, and no choledocholithiasis (Figure 1B). She proceeded to operating theater for a laparoscopic cholecystectomy during the same admission. The operative note states a large gallbladder with severe wall thickening and at least four large gallstones. There was a spillage of stones and, given their size, required four separate retrieval bags to remove them. The gallbladder was elongated and adherent to the cecum and ascending colon. Intraoperative cholangiogram demonstrated free contrast flow into the duodenum without evidence of retained stones, fistula, or dilated biliary ducts. The patient had a routine recovery post-operatively and was discharged home with a plan for follow-up CT adrenal protocol in two months to evaluate the incidental adrenal lesion.
The patient underwent a routine CT adrenal protocol in October 2016 with a finding of a stable indeterminant right adrenal lesion. On the same CT, a 31 mm unretrieved spilled gallstone in the upper abdomen just anterior to the stomach post-cholecystectomy (Figure 2A). The patient was advised by phone clinic for a repeat CT in 12 months to monitor the adrenal lesion. The reported gallstone was not acknowledged at the time. The follow-up CT adrenal protocol in August 2017 again reported a 31 mm calcified gallstone abutting the anterior wall of the gastric antrum similar in appearance to the previous CT (Figure 2B). The adrenal lesion remained stable and hence the patient was discharged from surgical follow-up.
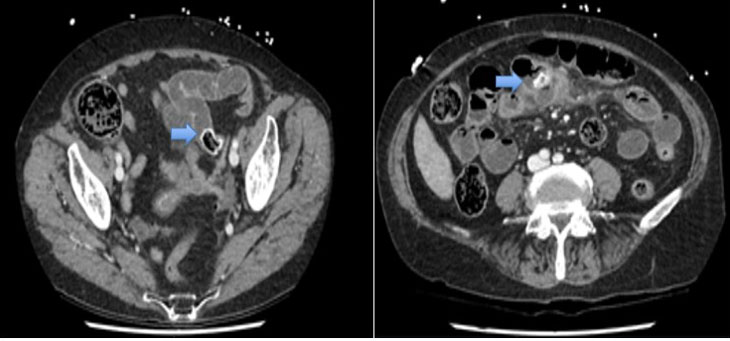
Six years later, in July 2022, the patient presented to the emergency department with a two-day history of abdominal pain, constipation, and vomiting. On examination, the vital signs were within the normal range and an abdominal examination revealed a distended but soft abdomen with tenderness in the lower abdomen. Blood tests revealed a slight elevation in white cell count (13.0×E9/L) and C-reactive protein (CRP) (14 mg/L). With clinical concern for a bowel obstruction, she proceeded for an abdominal X-ray, which showed dilated small bowel loops. A subsequent CT scan confirmed a small bowel obstruction due to gallstone ileus from a 31 mm intraluminal gallstone in the distal small bowel (Figure 3). On review of prior imaging, the gallstone was similar in appearance to the previously reported spilled peritoneal gallstone. There was no radiological evidence of pneumobilia to suggest a biliary-enteric fistula.
The patient was managed as a small bowel obstruction due to gallstone ileus. She had a nasogastric tube placed for decompression and eventually proceeded for a laparotomy. During laparotomy, a transition point for obstruction was in the terminal ileum where the gallstone was located. There was no concern for bowel ischemia or necrosis so a longitudinal enterotomy was performed to retrieve the gallstone (Figure 4). The enterotomy was then closed in a transverse fashion with interrupted 3-0 PDS sutures. The remainder of the bowel and stomach was carefully inspected for an obvious point of entry; however, this was not seen. She had a routine post-operative recovery and was discharged home after 8-day admission to the hospital (Figure 5).
Discussion
During routine laparoscopic cholecystectomy, approximately 5–40% of procedures are associated with spillage of gallstones [3],[4]. Traditionally, spillage of gallstones is not considered a significant concern as the documented complications from retained stones are rare [4]. The standard of teaching includes methods to reduce the risk of gallstone spillage, such as careful dissection, retraction, and bile aspiration [5]. If stones are spilled, then an attempt to retrieve the stones should be made if this is feasible to do so; however, particularly in a laparoscopic approach, this can be difficult. It is recommended to utilize copious irrigation to dilute any infected bile and attempt retrieval with retrieval bags if able [5]. Conversion to an open operation for retrieval of stones has been deemed unnecessary, given how rare complications from spilled stones are [6].
Although complications from unretrieved gallstones are rare, there is a variety of post-operative complications described in the literature, including intra-abdominal and subcutaneous abscess formation, abdominal mass, fistula formation, and fevers or bacteremia [7]. However, most complications occur within the first few months and can occur even up to 10 years after the procedure [8]. If complications arise, they may lead to significant morbidity and management may result in an invasive intervention, including a laparotomy [9].
Gallstone ileus is a rare complication of gallstone disease. Patients usually present with symptoms of bowel obstruction, and CT imaging shows the point of obstruction to be a gallstone with evidence of pneumobilia; this is known as Rigler’s Triad [10]. Typically, the etiology of this condition is in the context of a biliary-enteric fistula which may form due to a previous inflammatory process in the right upper quadrant, such as cholecystitis, cholangitis, diverticulitis, or gastrointestinal malignancy [11]. The most frequently seen fistula is a cholecystoduodenal fistula, followed by cholecystocolonic fistula and cholecystoduodenocolonic fistula [12]. In the absence of a biliary-enteric fistula, this condition is rarely seen.
We report a case of a patient with gallstone ileus several years following a laparoscopic cholecystectomy that involved spillage of multiple gallstones. Although retrieval of some stones occurred intraoperatively, the follow-up CT imaging obtained for the purposes of an adrenal lesion had identified a remaining spilled gallstone abutting the gastric antrum. Six years later, when the patient presented to hospital with gallstone ileus, the CT obtained shows this same gallstone was intraluminal in the distal small bowel, causing obstruction. Although an obvious point of entry was not seen intraoperatively, one can assume the gallstone had likely eroded through the stomach or bowel wall to migrate intraluminal. The absence of pneumobilia indicates that a biliary-enteric fistula is not present and the absence of intra-abdominal free air shows this migration has likely occurred over a long period of time.
Very few cases of gallstone ileus are identified in cholecystectomized patients in the absence of a fistula. Narasimhan et al. describe a case of gallstone ileus as a rare complication following an endoscopic retrograde cholangiopancreatography (ERCP) [13]. Draganic et al. and Zamora et al. describe cases of a gallstone eroding through the bowel wall only a few months following a laparoscopic cholecystectomy with spilled stones [14],[15]. Habib et al. describe an unusual case of a spilled gallstone that had eroded through a Meckel’s diverticulum [16]. In each of these cases, the stone appears to precipitate an inflammatory reaction adjacent to the bowel wall, and subsequently, enter the lumen to cause an obstruction.
Initial treatment of gallstone ileus involves stabilization and decompression with a nasogastric tube. Ultimately surgical intervention is pertinent for removal of the gallstone to resolve the obstruction [17]. An open or laparoscopic approach identifies the point of obstruction, and the gallstone can be retrieved through an enterotomy. Simple enterolithotomy with primary closure has been shown to resolve obstruction and have low post-operative complications [18]. A bowel resection may be considered if there is a concern for bowel ischemia or necrosis. There is no clear consensus on whether concurrent cholecystectomy and closure of the fistula, if present, should be performed during the same operation [19].
Conclusion
Gallstone ileus is a rare but serious complication of gallstone disease, with increased mortality rates due to delayed diagnosis. Although spillage of gallstones is common during cholecystectomy, traditionally it is not considered significant, as documented complications from retained stones are rare. This case demonstrates that gallstone ileus may present due to unretrieved spilled gallstones during a routine cholecystectomy. There can be a significant delay in presentation of gallstone ileus, in this case, six years after her initial cholecystectomy. During routine laparoscopic cholecystectomy, priority should be made to reduce risk of spilled stones with careful dissection, retraction, and bile aspiration. If spillage occurs, then retrieval should be attempted if feasible to do so. This case highlights the importance of recognizing and documenting spilled gallstones intraoperatively and if seen on subsequent imaging studies as they may lead to complications in the future.
REFERENCES
1.
Ayantunde AA, Agrawal A. Gallstone ileus: Diagnosis and management. World J Surg 2007;31(6):1292–7. [CrossRef]
[Pubmed]

2.
Raiford TS. Intestinal obstruction due to gallstones (Gallstone ileus). Ann Surg 1961;153(6):830–8. [CrossRef]
[Pubmed]

3.
Schäfer M, Suter C, Klaiber C, Wehrli H, Frei E, Krähenbühl L. Spilled gallstones after laparoscopic cholecystectomy. A relevant problem? A retrospective analysis of 10,174 laparoscopic cholecystectomies. Surg Endosc 1998;12(4):305–9. [CrossRef]
[Pubmed]

4.
Memon MA, Deeik RK, Maffi TR, Fitzgibbons RJ Jr. The outcome of unretrieved gallstones in the peritoneal cavity during laparoscopic cholecystectomy. A prospective analysis. Surg Endosc 1999;13(9):848–57. [CrossRef]
[Pubmed]

5.
Sathesh-Kumar T, Saklani AP, Vinayagam R, Blackett RL. Spilled gall stones during laparoscopic cholecystectomy: A review of the literature. Postgrad Med J 2004;80(940):77–9. [CrossRef]
[Pubmed]

6.
Demirbas BT, Gulluoglu BM, Aktan AO. Retained abdominal gallstones after laparoscopic cholecystectomy: A systematic review. Surg Laparosc Endosc Percutan Tech 2015;25(2):97–9. [CrossRef]
[Pubmed]

7.
Helme S, Samdani T, Sinha P. Complications of spilled gallstones following laparoscopic cholecystectomy: A case report and literature overview. J Med Case Rep 2009;3:8626. [CrossRef]
[Pubmed]

8.
Chowbey PK, Goel A, Bagchi N, et al. Abdominal wall sinus: An unusual presentation of spilled gallstone. J Laparoendosc Adv Surg Tech A 2006;16(6):613–5. [CrossRef]
[Pubmed]

9.
Yethadka R, Shetty S, Vijayakumar A. Attitudes and practices of surgeons towards spilled gallstones during laparoscopic cholecystectomy: An observational study. Int Sch Res Notices 2014;2014:381514. [CrossRef]
[Pubmed]

10.
Lassandro F, Gagliardi N, Scuderi M, Pinto A, Gatta G, Mazzeo R. Gallstone ileus analysis of radiological findings in 27 patients. Eur J Radiol 2004;50(1):23–9. [CrossRef]
[Pubmed]

11.
Savvidou S, Goulis J, Gantzarou A, Ilonidis G. Pneumobilia, chronic diarrhea, vitamin K malabsorption: A pathognomonic triad for cholecystocolonic fistulas. World J Gastroenterol 2009;15(32):4077–82.
[Pubmed]

12.
Clavien PA, Richon J, Burgan S, Rohner A. Gallstone ileus. Br J Surg 1990;77(7):737–42. [CrossRef]
[Pubmed]

13.
Narasimhan V, Ooi G, Loh D. Gallstone ileus following therapeutic endoscopic retrograde cholangiopancreatography. ANZ J Surg 2018;88(7–8):799–800. [CrossRef]
[Pubmed]

14.
Draganic BD, Reece-Smith H. Gallstone ileus without a gallbladder. Ann R Coll Surg Engl 1997;79(3):231–2.
[Pubmed]

15.
Zamora A, Chang J, Matsushima K. Progressive abdominal pain following laparoscopic cholecystectomy. JAMA Surg 2016;151(9):871–2. [CrossRef]
[Pubmed]

16.
Habib E, Elhadad A. Digestive complications of gallstones lost during laparoscopic cholecystectomy. HPB (Oxford) 2003;5(2):118–22. [CrossRef]
[Pubmed]

17.
Alemi F, Seiser N, Ayloo S. Gallstone disease: Cholecystitis, Mirizzi syndrome, Bouveret syndrome, Gallstone ileus. Surg Clin North Am 2019;99(2):231–44. [CrossRef]
[Pubmed]

18.
Dreifuss NH, Schlottmann F, Cubisino A, Mangano A, Baz C, Masrur MA. Totally laparoscopic resolution of gallstone ileus: A case report. Int J Surg Case Rep 2022;90:106682. [CrossRef]
[Pubmed]

19.
Vera-Mansilla C, Sanchez-Gollarte A, Matias B, Mendoza-Moreno F, Díez-Alonso M, Garcia-Moreno Nisa F. Surgical treatment of gallstone ileus: Less is more. Visc Med 2022;38(1):72–7. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Binura Buwaneka Wijesinghe Lekamalage - Conception of the work, Design of the work, Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Prasanthan Thaveenthiran - Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Kaustubha Nikhil Ghate - Drafting the work, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Asiri Arachchi - Conception of the work, Design of the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2023 Binura Buwaneka Wijesinghe Lekamalage et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.