|
Case Report
A challenging entity for endocrine surgeons: Ectopic lingual thyroid gland. A case-based update
1 MD, UOC Multifunctional Center of Endocrine Surgery, Cristo Re General Hospital, Rome, Italy
2 MD, Department of General Surgery, University of Rome “Tor Vergata”, Rome, Italy
3 MD, Division of Otorinolaringology, Cristo Re General Hospital, Rome, Italy
4 MD, UOC of Radiology, Section of Nuclear Medicine, Cristo Re General Hospital, Rome, Italy
5 UOC of Radiology, Cristo Re General Hospital, Rome, Italy
6 MD, Unicamillus International Medical University, Rome, Italy
Address correspondence to:
Pietro Princi
Chief, Multifunctional Center of Endocrine Surgery, Cristo Re General Hospital, via delle Calasanziane 25, 00168 Rome,
Italy
Message to Corresponding Author
Article ID: 100151Z12ST2025
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Tempera SE, Nigro C, D’Ottavi LR, Ieria FP, Perrone L, Princi P. A challenging entity for endocrine surgeons: Ectopic lingual thyroid gland. A case-based update. J Case Rep Images Surg 2025;11(1):13–18.ABSTRACT
Introduction: Lingual thyroid (LT) is a rare embryologic anomaly. Diagnosis is challenging and treatment is still controversial.
Case Report: We report a case of a 46 years old man with occasional sore throat, who underwent an otorhinolaryngology evaluation. Fiber optic flexible indirect laryngoscopy (FIL) highlighted a mass at the base of the tongue. Subsequent surgeon-performed neck ultrasound, computed tomography (CT) scan and thyroid scintiscan confirmed the diagnosis of LT. The patient had never investigated the thyroid before as he was totally asymptomatic. Subsequent blood tests revealed subclinical hypothyroidism. Fine needle aspiration (FNAC) showed benign cytology. After a multidisciplinary discussion, the patient was treated with suppressive doses of thyroxine due to subclinical hypothyroidism. At the follow-up the patient showed a size reduction of the ectopic gland at ultrasound and resolution of the initial symptoms.
Conclusion: A comprehensive pertinent literature review was performed, showing few small series of patients affected by LT. Treatment options proposed for LT include thyroid hormone suppression therapy, radioactive iodine (RAI) ablation, and surgical excision. However, a consensus in management does still not exist so far. Most authors agree that no treatment is required when LT is asymptomatic and the patient is euthyroid. Thus, we proposed an update of the diagnostic and therapeutic algorithm for the management of LT based on the present cases. Further research regarding evaluation, monitoring and follow-up of ectopic thyroid tissue is necessary for better assessment of the workup and management of LT, in particular due to its possible but rare malignant nature.
Keywords: Lingual thyroid, Therapeutic algorithm, Thyroid ectopy, Thyroid surgery
Introduction
Lingual thyroid (LT) is a rare congenital anomaly involving the migration of the thyroid gland through the neck (from the foramen cecum to its usual pre-laryngeal location), which results as an ectopic gland localized at the base of the tongue, usually situated in the midline [1].
While the findings of thyroglossal duct cysts with residue of thyroid tissues represent the most common congenital mass of the midline of the neck, the base of the tongue is the most frequent site for a whole ectopic thyroid gland [2],[3]. In most of LT cases (around 70%), the orthotopic gland tissue is absent [3],[4].
The prevalence varies between 1:100,000 and 1:300,000, and the incidence has been reported to be between 1 in 300 and 1 in 100,000 population, with a female predominance [4],[5],[6], but probably the true incidence is underestimated due to its asymptomatic behavior [7]. In fact, many patients remain asymptomatic throughout life, while some patients may refer nonspecific symptoms such as discomfort, dysphagia, dyspnea, or vocal alterations. Some cases are discovered incidentally during imaging studies performed for other reason [3],[5],[6].
A pre-treatment consensus on diagnostic algorithm does still not exist, due to its rare presentation. In case of clinical suspicion for LT, some authors recommend second level exams like computed tomography (CT) scan or magnetic resonance (MR) examination. A thyroid scintigraphy scan is necessary to asses if the diagnosticated mass is the only functional thyroid tissue present [6],[8]. Thyroid function examinations are mandatory. Blood tests of these patients reveal a normal function in most of cases. Sometimes patients present hypothyroidism, while rare cases of hyperthyroidism have been reported [4],[9]. The onset of thyroid carcinoma is rare, with an estimated incidence of 1% [10],[11], but the diagnosis of malignancy could be challenging. Indeed, some authors affirm that benign LT and malignant LT are indistinguishable clinically and radiographically, so that at least a cytology determination is recommended [1],[2],[8].
Principal treatment options for LT include thyroid hormone suppression therapy, radioactive iodine (RAI), and surgical excision [4],[11],[12], which could turn out very challenging, due to the anatomical relationships with the surrounding vascular and nervous structures [4]. There have been proposals for the ablation of the mass with radiofrequency or thermal ablation, however, data on the results are still lacking [13],[14]. However, a consensus in management and treatment of LT has not yet been formulated.
A case of LT came to our attention in December 2022. Thereafter, a narrative review of the literature and an update of the workup and management of this rare entity were performed.
Case Report
We report a case of a 46 years old man, asymptomatic till that day, who underwent an otolaryngology evaluation for occasional sore throat. The patient reported no comorbidity and was not taking any type of home drug therapy.
Fiber optic flexible indirect laryngoscopy (FIL) revealed a mass at the base of the tongue, thus arising the diagnostic suspicion of LT. The diagnosis was confirmed by an endocrine surgeon-performed neck ultrasound that revealed a 34 mm solid hypoechoic slightly heterogeneous suprahyoid nodular structure compatible with thyroid tissue. No thyroid parenchyma was detectable in the usual thyroid site. No pathologic lymph nodes were detectable (Figure 1).
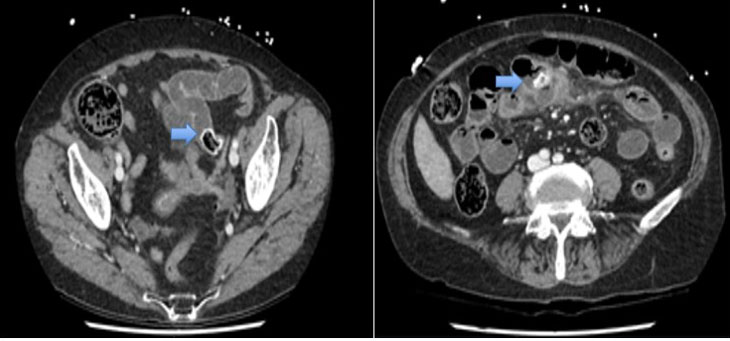
Computed tomography scan documented a non-homogeneously hyperdense structure with an oval morphology of 25 mm with a craniocaudal extension of 29 mm that is located behind the base of the tongue and above the hyoid bone and the epiglottis with which it contracts continuity. No thyroid was appreciable in its normal anatomical location (Figure 2).
The Tc99 scan investigation (TC99M *I, 72 MBq, i.v.) highlighted increased tracer uptake consistently with the structure reported on ultrasound imaging. Uptake in the anterior region of the neck and in other areas of the body was absent (Figure 3).
The patient had never investigated the thyroid before as he was totally asymptomatic. Subsequent blood tests revealed subclinical hypothyroidism: thyroid-stimulating hormone (TSH) 6.63 uIU/mL (range 0.4–4.00), normal FT3, FT4, negative antibodies, normal level of calcitonin, and intact parathyroid hormone (i-PTH).
Fine needle aspiration was performed and showed benign thyroid tissue without evidence of atypia (TIR2–SIAPEC 2014) [15].
After a multidisciplinary discussion, involving endocrinologist, endocrine surgeons, otolaryngologist, and radiologists, the patient was treated with increasing suppressive doses of thyroxine, due to subclinical hypothyroidism. At the 6-month follow-up, the patient showed a normalization of thyroid function, without presenting side effects related to suppressive therapy. At the latest follow-up, which is after one year of therapy, the patient reported complete remission of the initial symptoms and ultrasounds showed slight reduction in size of the ectopic tissue (29 mm vs 34 mm of the maximum diameter).
Thus, the multidisciplinary board decided to continue a yearly follow-up and to modify the therapeutic strategy only in case of failure of the current one, namely increasing size of the LT and/or new onset of symptoms.
Discussion
Lingual thyroid (LT) is a rare congenital anomaly. It represents the most frequent site of thyroid ectopia (almost 90%), although we can also find thyroid tissue in other regions, such as the lateral cervical region, trachea, submandibular area, antero-superior mediastinum, etc., or outside the neck (e.g., axillary, breast, and eye) [4]. An involvement of some genetic alterations of transcription factors like TITF-1, PAX8, and Foxe1 has been supposed to cause an abnormal migration of the gland [16],[17].
First case of LT ectopia was described in 1869 by Hickman, reporting a case report of newborn death caused by suffocation for a huge thyroid mass located at the base of the tongue [18]. Our review of the literature shows very few case series, with case reports including 1 to 3 patients most frequently published. The largest case series comes from the Mayo Clinic, Rochester, Minnesota with a first paper reporting 15 patients treated from 1907 to 1971 [19] and a more recent paper authored by Carranza Leon et al. in 2016, including 29 cases treated in the period 1976–2010 [6]. In 1979, Kamat et al. [20] reported a series of 12 patients treated at Tata Memorial Hospital, Bombay India. In 2023, Gao et al. reported a large series of 47 patients treated for ectopic thyroid, including 20 cases of LT [21]. The prevalence reported in literature varies between 1:100,000 and 1:300,000 and the incidence has been reported to be between 1 in 300 and 1 in 100,000 population, with a female predominance (5:1) [4],[5],[6],[19],[22],[23]. The age at the diagnosis varies significantly in the literature, partially depending on different national settings. Parida et al. [24] reported a mean age of eight years in children (range 6–11) and 28.7 years in adult patients (range 18–43). In the large series reported by Carranza Leon et al. [6] around 32% of LT were detected during puberty and adolescence, while other study reported different percentage (45.1%) [25]. Actually, the real incidence and prevalence are probably underestimated due to its asymptomatic behavior [7]. As we described previously, many patients remain asymptomatic throughout life, while some patients may refer nonspecific symptoms, as in the present case. Some cases are diagnosed incidentally during imaging studies like CT scan or MR performed for other reason, as described by Altay et al. [3].
Due to its rare presentation, there is not a final consensus on diagnostic algorithm so far.
After literature review [4],[5],[6],[22],[24],[26], our attitude is that in case of suspected diagnosis of LT, at least an ultrasound (US) of the neck must be performed. Ultrasound may exclude suspicious features, the presence of suspicious lymph nodes in the anterior or lateral cervical region, and the presence of further thyroid tissue in both typical and non-typical locations in the neck. We recommend to perform second level exams like CT scan or MR for a better definition of the lesion in terms of vascularization, relationships with surrounding structures, and to exclude any infiltration of these structures. Thyroid scintigraphy is necessary to confirm the LT diagnosis and to assess if the diagnosed mass is the only functional thyroid tissue present. The assessment of thyroid function is necessary for decision-making treatment after diagnosis. We suggest to perform TSH, FT3, and FT4 blood test and to dose circulating antibodies to thyroid antigens (mainly thyro-peroxidase and thyroglobulin) and calcitonin, in order to rule out thyroiditis or rare carcinoma. As we previously described, the onset of thyroid carcinoma is rare, but the diagnosis of malignancy could be challenging. In 2001, Massine et al. [27] affirmed that fewer than 30 cases of LT carcinoma had been reported in the literature. A more recent review performed by Vincent et al. [26] reports less than 60 cases of LT carcinoma published so far. These patients commonly present with symptoms (dyspnea, dysphagia, voice alteration, or bleeding). As in the normal thyroid, the most frequent histology subtype is papillary. Thus, LT carcinoma can be treated similarly to usual thyroid carcinoma, with optimal results after surgery and following RAI ablation, when necessary. Anyway, considering that the differential diagnosis between benign and malignant LT can be very challenging, either clinically and radiographically, we recommend FNAC determination of the lesion in any case of LT. Fine needle aspiration may give an inconclusive or non-diagnostic result. However, according to the literature [4],[5],[28],[29], as well as in our opinion, it may instead provide a valid support to drive the subsequent therapeutic decision. Our proposed diagnostic management is summarized in Table 1.
As widely underlined, the cases of LT described in the literature are few. For this reason, there is no univocal consensus on the treatment. Some authors state that surgery is the first treatment of choice, also considering the possible malignant nature of the mass [29],[30]. Actually, most of authors agree on a more conservative attitude, designing a treatment tailored to the patient.
Some authors had even proposed a more structured treatment algorithm [6],[24]. The authors agree that no treatment is required in asymptomatic and euthyroid patients. Thus, in asymptomatic patients, eventual treatment is based on thyroid function: no treatment is required if euthyroid, if hypothyroid thyroid hormone replacement is the treatment of choice. Obviously, these patients need periodic clinical evaluation and blood tests. If symptoms increase, it will be necessary to re-evaluate the case and proceed with more effective treatments.
In case of mild symptoms reported by the patient, suppressive therapy with thyroid hormones can be proposed in order to reduce the mass. In the event of failure of suppressive therapy or in case of patients with severe symptoms, such as airways obstruction, the surgical option should be evaluated. Surgery should aim at the total removal of the mass in order to avoid recurrences, although some authors also propose partial resections in selected cases [22]. The most frequent surgical approaches proposed in the literature are:
- Transoral approach is indicated in case of small masses. It greatly reduces morbidity and complications related to deep neck structures lesions (fistula formation, deep cervical infections, or lingual nerve injury). On the other hand, minimal exposure of the operating field can more easily cause lingual artery injury with consequent hemorrhage and difficulty in managing it [6],[12],[26].
- External approach, such as lateral pharyngectomy, is more suitable in case of large masses. It warrants a wide visualization of the operating field and surrounding structures, allowing better control in case of hemorrhage, but is also associated with a higher incidence of complications such as fistula, deep neck infections, as well as giving the patient a noticeable scar [6],[12].
Microinvasive surgical treatments have also been proposed and are being introduced (such as transoral laser microsurgery and ultrasonic transoral resection), as well as RAI treatment or radiofrequency ablation has been proposed as valid alternatives to surgery, when it is precluded for morbidity or declined by the patient. The RAI therapy reduces the size of the lesion producing fibrosis and degeneration of the up-taking ectopic thyroid tissue [1]. Similarly, radiofrequency ablation reduces the size of the mass causing a coagulative necrosis by disrupting cellular integrity, which later leads into tissue contraction and size reduction of the mass [13],[14].
The airway management deserves an important mention both in the case of more conservative treatments and in the case of surgery. Significant edema of the post-treatment structures may occur and can cause severe obstructive symptoms that must be promptly treated. Some authors more cautiously recommend evaluating a temporary tracheostomy or a 24 hours intubation after surgery [22]. Other authors instead recommend only having everything necessary for urgent reintubation available at the bedside and a tracheostomy tray in case of need [12].
Conclusion
Our case shows how conservative management with suppressive doses of thyroxine resulted in reduction of the LT size end reduction of symptoms, avoiding unnecessary surgical intervention, which could potentially lead to severe complication. Diagnosis of LT could be challenging but is mandatory to tailor the correct treatment. We highly suggest a multidisciplinary approach including endocrinologist, endocrine surgeon, otolaryngologist, radiologist, and anesthesiologist to better define the correct patient management. Cooperative studies are advocated to further refine the assessment and management of ectopic thyroid tissue and LT more specifically, due to its possible rare malignant nature.
REFERENCES
1.
Ibrahim NA, Fadeyibi IO. Ectopic thyroid: Etiology, pathology and management. Hormones (Athens) 2011;10(4):261–9. [CrossRef]
[Pubmed]

2.
Noussios G, Anagnostis P, Goulis DG, Lappas D, Natsis K. Ectopic thyroid tissue: Anatomical, clinical, and surgical implications of a rare entity. Eur J Endocrinol 2011;165(3):375–82. [CrossRef]
[Pubmed]

3.
Altay C, Erdoğan N, Karasu S, et al. CT and MRI findings of developmental abnormalities and ectopia varieties of the thyroid gland. Diagn Interv Radiol 2012;18(4):335–43. [CrossRef]
[Pubmed]

4.
Guerra G, Cinelli M, Mesolella M, et al. Morphological, diagnostic and surgical features of ectopic thyroid gland: A review of literature. Int J Surg 2014;12 Suppl 1:S3–11. [CrossRef]
[Pubmed]

5.
Santangelo G, Pellino G, De Falco N, et al. Prevalence, diagnosis and management of ectopic thyroid glands. Int J Surg 2016;28 Suppl 1:S1–6. [CrossRef]
[Pubmed]

6.
Carranza Leon BG, Turcu A, Bahn R, Dean DS. Lingual thyroid: 35-year experience at a tertiary care referral center. Endocr Pract 2016;22(3):343–9. [CrossRef]
[Pubmed]

7.
Sauk JJ Jr. Ectopic lingual thyroid. J Pathol 1970;102(4):239–43. [CrossRef]
[Pubmed]

8.
Wong RJ, Cunningham MJ, Curtin HD. Cervical ectopic thyroid. Am J Otolaryngol 1998;19(6):397–400. [CrossRef]
[Pubmed]

9.
Jacob MJ, Ravina M. A rare case of lingual thyroid with hyperthyroidism: A case report and review of the literature. Indian J Endocrinol Metab 2012;16(3):441–3. [CrossRef]
[Pubmed]

10.
Falvo L, Berni A, Catania A, D’Andrea V, Palermo S, Giustiniani C, De Antoni E. Sclerosing papillary carcinoma arising in a lingual thyroid: Report of a case. Surg Today 2005;35(4):304–8. [CrossRef]
[Pubmed]

11.
Klubo-Gwiezdzinska J, Manes RP, Chia SH, et al. Clinical review: Ectopic cervical thyroid carcinoma—Review of the literature with illustrative case series. J Clin Endocrinol Metab 2011;96(9):2684–91. [CrossRef]
[Pubmed]

12.
Jabbour J, Agostinho N, Bains HK, et al. Lump at the back of my tongue. The lingual thyroid – A case report and narrative review of literature. Clin Case Rep 2021;9(6):e04160. [CrossRef]
[Pubmed]

13.
Dasari SD, Bashetty NK, Prayaga NSM. Radiofrequency ablation of lingual thyroid. Otolaryngol Head Neck Surg 2007;136(3):498–9. [CrossRef]
[Pubmed]

14.
Cunningham CL, Vilela RJ, Roy S. Radiofrequency ablation as a novel treatment for lingual thyroid. Int J Pediatr Otorhinolaryngol 2011;75(1):137–9. [CrossRef]
[Pubmed]

15.
Nardi F, Basolo F, Crescenzi A, et al. Italian consensus for the classification and reporting of thyroid cytology. J Endocrinol Invest 2014;37(6):593–9. [CrossRef]
[Pubmed]

16.
Gillam MP, Kopp P. Genetic regulation of thyroid development. Curr Opin Pediatr 2001;13(4):358–63. [CrossRef]
[Pubmed]

17.
De Felice M, Di Lauro R. Thyroid development and its disorders: Genetics and molecular mechanisms. Endocr Rev 2004;25(5):722–46. [CrossRef]
[Pubmed]

18.
Waters ZJ, Mccullough K, Thomas NR. Lingual thyroid; historical data, developmental anatomy, and report of a case. AMA Arch Otolaryngol 1953;57(1):60–78 [CrossRef]
[Pubmed]

19.
Neinas FW, Gorman CA, Devine KD, Woolner LB. Lingual thyroid. Clinical characteristics of 15 cases. Ann Intern Med 1973;79(2):205–10. [CrossRef]
[Pubmed]

20.
Kamat MR, Kulkarni JN, Desai PB, Jussawalla DJ. Lingual thyroid: A review of 12 cases. Br J Surg 1979;66(8):537–9. [CrossRef]
[Pubmed]

21.
Gao M, He Q, Li L, et al. The clinicopathological features, treatment outcomes and follow-up results of 47 ectopic thyroid gland cases: A single-center retrospective study. Front Endocrinol (Lausanne) 2023;14:1278734. [CrossRef]
[Pubmed]

22.
Toso A, Colombani F, Averono G, Aluffi P, Pia F. Lingual thyroid causing dysphagia and dyspnoea. Case reports and review of the literature. Acta Otorhinolaryngol Ital 2009;29(4):213–7.
[Pubmed]

23.
Williams JD, Sclafani AP, Slupchinskij O, Douge C. Evaluation and management of the lingual thyroid gland. Ann Otol Rhinol Laryngol 1996;105(4):312–6. [CrossRef]
[Pubmed]

24.
Parida PK, Herkel K, Preetam C, Pradhan P, Samal DK, Sarkar S. Management of lingual thyroid with second thyroid anomaly: An institutional experience. Indian J Otolaryngol Head Neck Surg 2022;74(Suppl 3):5329–37. [CrossRef]
[Pubmed]

25.
Baughman RA. Lingual thyroid and lingual thyroglossal tract remnants. A clinical and histopathologic study with review of the literature. Oral Surg Oral Med Oral Pathol 1972;34(5):781–99. [CrossRef]
[Pubmed]

26.
Vincent A, Jategaonkar A, Kadakia S, Ducic Y. TORS excision of lingual thyroid carcinoma: Technique and systematic review. Am J Otolaryngol 2019;40(3):435–9. [CrossRef]
[Pubmed]

27.
Massine RE, Durning SJ, Koroscil TM. Lingual thyroid carcinoma: A case report and review of the literature. Thyroid 2001;11(12):1191–6. [CrossRef]
[Pubmed]

28.
Cruz-Dardíz N, Rivera-Santana N, Torres-Torres M, et al. Lingual thyroid gland: It’s time for awareness. Endocrinol Diabetes Metab Case Rep 2020;2020:EDM20–0026. [CrossRef]
[Pubmed]

29.
Gotlib J, Ianessi A, Santini J, Dassonville O. Ectopic lingual thyroid. Eur Ann Otorhinolaryngol Head Neck Dis 2016;133(2):155–6. [CrossRef]
[Pubmed]

30.
Shah BC, Ravichand CS, Juluri S, Agarwal A, Pramesh CS, Mistry RC. Ectopic thyroid cancer. Ann Thorac Cardiovasc Surg 2007;13(2):122–4.
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Serena Elisa Tempera - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Casimiro Nigro - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Luigi Raimondo D’Ottavi - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Francesco Pio Ieria - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Luca Perrone - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Pietro Princi - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2025 Serena Elisa Tempera et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.