|
Case Report
A rare complication of jejunal diverticulae resulting in a closed loop bowel obstruction
1 General Surgery Department, Canberra Hospital, Australian Capital Territory, Australia
Address correspondence to:
Zen Zuan Yong
General Surgery Department, Canberra Hospital, Australian Capital Territory,
Australia
Message to Corresponding Author
Article ID: 100165Z12ZY2026
Access full text article on other devices

Access PDF of article on other devices

How to cite this article
Yong ZZ, Balasooriya J. A rare complication of jejunal diverticulae resulting in a closed loop bowel obstruction. J Case Rep Images Surg 2026;12(1):1–4.ABSTRACT
Jejunal diverticulosis (JD) is an uncommon and often underdiagnosed condition, usually discovered incidentally and rarely associated with acute complications such as diverticulitis, obstruction, abscess, perforation, or fistula formation. However, when complications do occur, they can be severe and diagnostically challenging. We present the case of a 75-year-old Female who arrived with an acute-onset abdominal pain with progressive distension and persistent vomiting. Computed tomography (CT) revealed a small bowel obstruction due to an enterolith. Emergency laparotomy revealed a small bowel obstruction at mid ileum due to an enterolith as well as an omental band adhered to the inflamed jejunal diverticulum proximally resulting in a closed loop in the affected segment of small bowel. The omental band was divided and the enterolith was removed via an enterotomy without requiring a small bowel resection. The patient was managed with antibiotics postoperatively and she made an unremarkable recovery. Closed loop small bowel obstruction as a result of complicated jejunal diverticular disease is rare in the literature and it highlights the critical importance of maintaining a high index of suspicion, particularly in older patients presenting with acute abdomen.
Keywords: Closed loop bowel obstruction, Jejunal diverticulae, Jejunal diverticulitis
Introduction
Small bowel diverticulosis was first described in 1794 by Sommering and further explored in 1807 by Sir Astley Cooper, with a reported incidence of up to 2.3% in autopsy and radiological studies. The condition is typically asymptomatic and most often identified incidentally on imaging [1]. Approximately 18% of cases develop acute complications, with around half of these requiring surgical intervention. Reported complications include diverticulitis, abscess formation, malabsorption, obstruction, perforation, and hemorrhage, occurring in up to 30% of patients, with mortality rates reaching 50% in severe cases [2]. There has been several case reports in which jejunal diverticulosis can cause a small bowel obstruction due to isolated enterolith or adhesion bands; however, this case report would be the first unique case of a closed loop small bowel obstruction from simultaneous omental band from an inflamed diverticulum as well as an enterolith intraluminally. Informed consent was obtained from the patient for publication.
Case Report
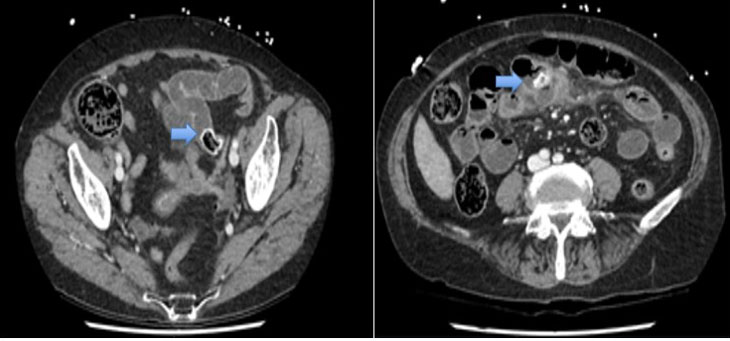
This 75-year-old female presented to a regional hospital and was subsequently transferred to our institution for assessment by the general surgical team. She was complaining of severe sudden onset abdominal pain for one day associated with multiple episodes of vomiting and had been getting worse. On examination she was hemodynamically stable and the abdomen was distended and diffusely tender. Biochemical markers were unremarkable. Subsequent CT scan revealed a jejunal diverticulitis with largest diverticulum containing a large mixed density structure, in keeping with an enterolith. The adjacent diverticulum no longer contained an enterolith which was seen on a previous CT (Figure 1). Evidence of small bowel obstruction noted with abrupt transition at the level of the left pelvic brim secondary to the migrated enterolith. Pelvic and interloop free fluid was also noted. She was managed with a nasogastric tube and fluid resuscitation and proceeded for an emergency laparotomy.
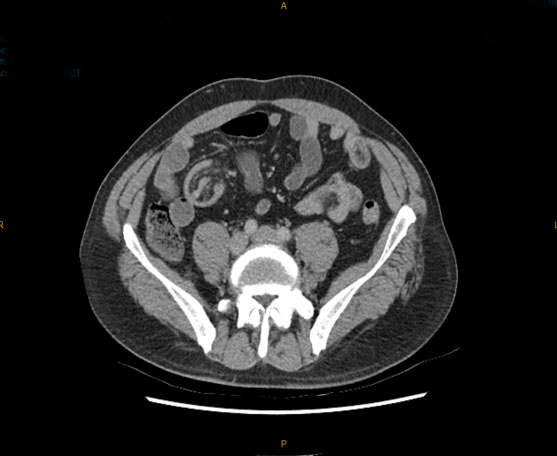
During the laparotomy, it was discovered that there was a distal small bowel obstruction from the enterolith at mid-ileal level and an omental band adhered to inflamed jejunal diverticulum proximally resulted in a closed loop bowel obstruction. This explained the rapid progression of symptoms. Obstructed segment of small bowel was viable and there were multiple other jejunal diverticulae noted. Dilation of jejunum proximal to the omental band also noted (Figure 2).
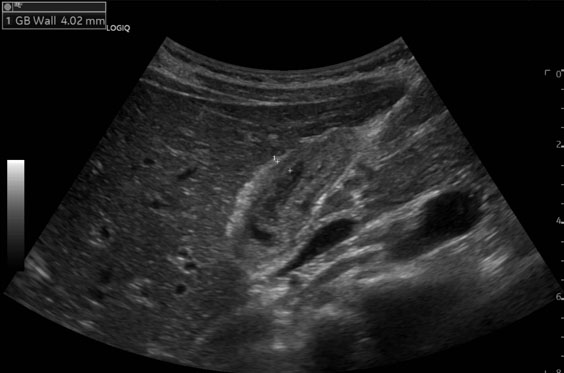
The band was divided and an enterotomy was performed proximal to obstruction site to remove the enterolith. The remaining enteroliths in the inflammed jejunal diverticulum as well as in the adjescent diverticulum was retrieved from the same enterotomy after fragmentation (Figure 3). The diverticulae were left intact and treated with intravenous antibiotics. The patient recovered well postoperatively without any significant complications.
Discussion
The clinical presentation for JD is rare, with reports of 0.3–2.3% in autopsy as well as radiologic series. The exact pathogenesis of this condition remains vague. However, it is thought to be the result from dysfunction of the smooth muscle layers or the myenteric plexus. This dysfunction leads to abnormal peristalsis leading to increased intraluminal pressure and hence the formation of diverticulum [3].
Obstruction secondary to jejunal diverticula is rare and most commonly occurs through mechanisms such as volvulus, entrapment of small bowel loops within a mesenteric diverticular sac, adhesions from chronic inflammation, or impaction of enteroliths formed within the diverticulum with very few isolated cases in the literature [4]. In such cases, delayed diagnosis may occur because clinical and radiologic findings are often nonspecific, and jejunal diverticula are frequently incidental or overlooked on imaging.
Management of complicated JD depends on clinical, biochemical, and radiological findings, ranging from conservative measures to small bowel resection. The enteroliths are thought to be formed within the diverticula of small bowel when contents become stagnant and stasis, leading to bacterial overgrowth and aggregation of choleric acids [5]. The management involving enterolith-related small bowel obstruction would be breaking down the enterolith and milking it into the colon. Conservative treatment if usually effective with enterotomies reserved for failed cases from conservative management [6]. The final decision to resect jejunal diverticulae would depend on the overall situation with resection more favored toward complicated diverticulosis whereas a simple enterolith removal is adequate for an initial obstruction from it [7].
When a small bowel resection and primary anastomosis is considered, only removal of the diverticulum bearing segment responsible for the obstruction while avoiding unnecessarily extensive resections is favored, given the potential for multifocal diverticulosis [8]. There has also been suggestion in the literature that all small bowel diverticula should be checked and all potential enteroliths removed to prevent any subsequent complications which we have done in our case.
Conclusion
The case presented highlights the importance of maintaining a high index of suspicion for complications of jejunal diverticulosis. Although rare and often clinically silent, JD can present with serious and potentially life-threatening complications. This case illustrates an exceptionally uncommon manifestation: a closed-loop small bowel obstruction caused by an enterolith intraluminally distally and a proximal omental band extraluminally. Early recognition, identification, and operative management is of utmost importance to reduce the risk of progression to perforation, ischemia, and sepsis. With this increase in awareness of the complications of JD, especially in patients’ with vague symptoms can help with improved patient outcomes.
REFERENCES
1.
Tsiotos GG, Farnell MB, Ilstrup DM. Nonmeckelian jejunal or ileal diverticulosis: An analysis of 112 cases. Surgery 1994;116(4):726–31; discussion 731–2.
[Pubmed]

2.
Falidas E, Vlachos K, Mathioulakis S, Archontovasilis F, Villias C. Multiple giant diverticula of the jejunum causing intestinal obstruction: Report of a case and review of the literature. World J Emerg Surg 2011;6(1):8. [CrossRef]
[Pubmed]

3.
Kouraklis G, Glinavou A, Mantas D, Kouskos E, Karatzas G. Clinical implications of small bowel diverticula. Isr Med Assoc J 2002;4(6):431–3.
[Pubmed]

4.
5.
Hofmann AF, Mysels KJ. Bile acid solubility and precipitation in vitro and in vivo: The role of conjugation, pH, and Ca2+ ions. J Lipid Res 1992;33(5):617–26.
[Pubmed]

6.
Gurvits GE, Lan G. Enterolithiasis. World J Gastroenterol 2014;20(47):17819–29. [CrossRef]
[Pubmed]

7.
Harris LM, Volpe CM, Doerr RJ. Small bowel obstruction secondary to enterolith impaction complicating jejunal diverticulitis. Am J Gastroenterol 1997;92(9):1538–40.
[Pubmed]

8.
Palder SB, Frey CB. Jejunal diverticulosis. Arch Surg 1988;123(7):889–94. [CrossRef]
[Pubmed]

SUPPORTING INFORMATION
Author Contributions
Zen Zuan Yong - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Janaka Balasooriya - Conception of the work, Design of the work, Acquisition of data, Analysis of data, Drafting the work, Revising the work critically for important intellectual content, Final approval of the version to be published, Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
AcknowledgmentsThis work has utilized the ChatGPT (GPT-5.1 model), developed by OpenAI, for assistance with language refinement and organization for fine tuning sentence structures.
Guarantor of SubmissionThe corresponding author is the guarantor of submission.
Source of SupportNone
Consent StatementWritten informed consent was obtained from the patient for publication of this article.
Data AvailabilityAll relevant data are within the paper and its Supporting Information files.
Conflict of InterestAuthors declare no conflict of interest.
Copyright© 2026 Zen Zuan Yong et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information.